Surviving the 2026 Heatwave: How Extreme Heat Triggers Muscle Cramps and Joint Pain

The Pakistan Meteorological Department has just issued its starkest warning to date: the Super El Niño of 2026 is on track to drive Karachi’s surface temperature past 50°C for several consecutive days. This is not a weather event. That is a physiological emergency, arriving in waves, claiming the first victims from among the weakest - the elderly, the hypertensive, the arthritic, the millions of office workers and labourers who will sweat through four-hour power outages with no relief. Every doctor in this city is rightly anticipating heatstroke. But what they will not be treating - the injuries that will quietly paralyse households for weeks after the fever breaks - are the agonising muscle cramps, the swollen joints that refuse to bend, the lower backs that have seized into rigid concrete. That is where physiotherapy begins - and that is what this article is about.
I see it every summer in my home visits across Karachi's popular areas. I walk into a patient’s flat and their calf is still in a hard knot from the cramp that woke them screaming at 2 AM. Their knee is hot to the touch and grinding on every step - not infected, just brutally dehydrated and irritated. Their lower back is so locked they cannot rotate to reach for a glass of water. These are not separate problems. They are all one systemic failure: a dehydrated, electrochemically bankrupt musculoskeletal system being asked to function under 45°C of thermal stress without adequate intervention. What does most of the city do? It takes a painkiller and blasts the AC at 16°C. Both responses make things materially worse, and I will explain exactly why.
This is a clinical preventative education piece, not a substitute for emergency services. If you are confused, have stopped sweating, have a core body temperature above 40°C, or have lost consciousness, you have heatstroke and need the emergency department immediately. What follows is for the tens of thousands who survive the heat but are left with a musculoskeletal system in ruins - and who need a clear, biomechanically grounded plan to get their bodies back.
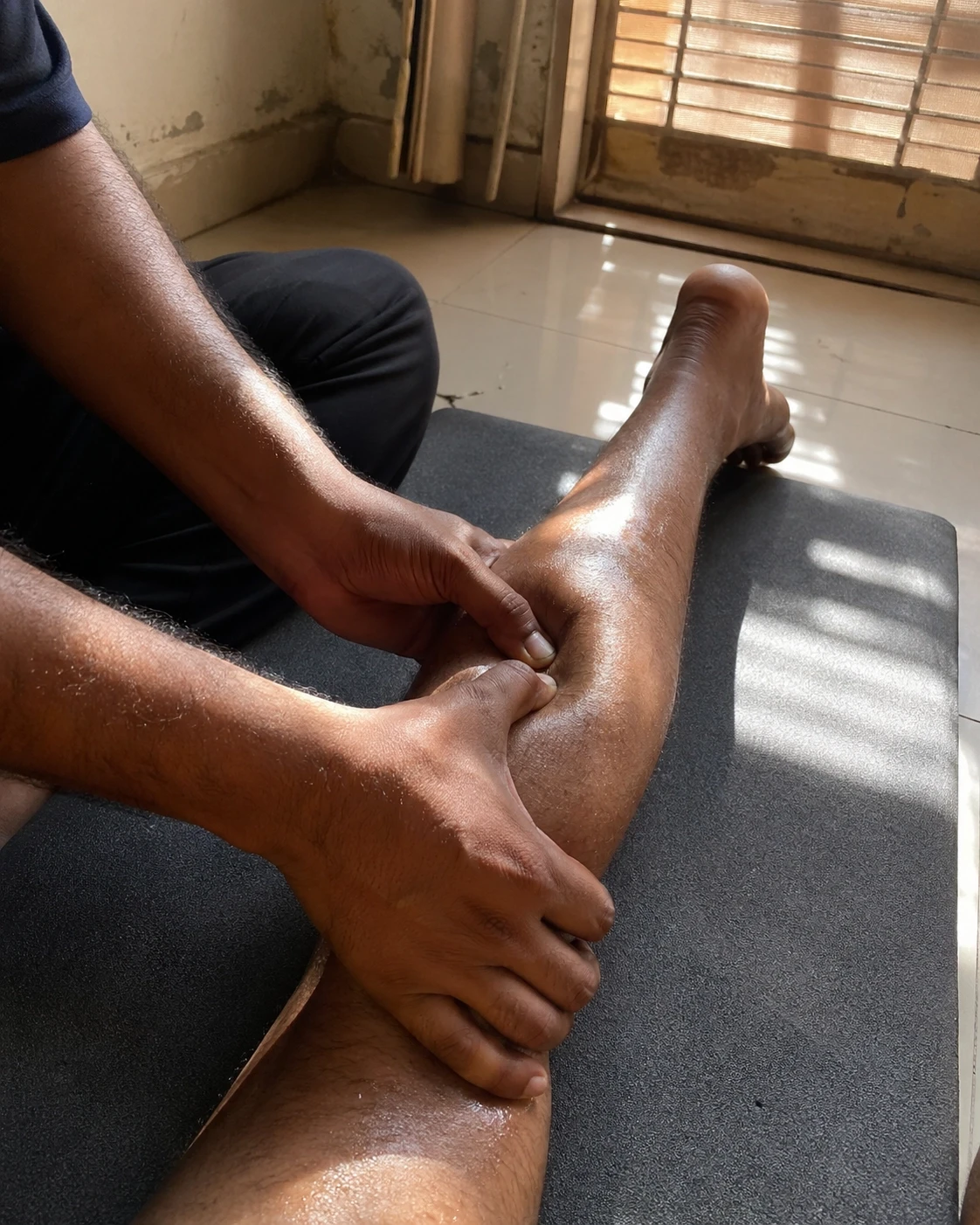
Quick Action Reference: What Your Body Is Actually Telling You
Before we go deep into the biomechanics, here is the fastest way to understand what these symptoms mean - and where most people go catastrophically wrong.
The Physical Symptom | The Biomechanical Reality | The Fatal Mistake |
Sudden nocturnal calf cramps | Hyponatremia-induced involuntary tetanic contraction - sodium-depleted sarcoplasmic reticulum cannot release calcium from the cross-bridge cycle, leaving the muscle fibre locked in contraction. | Violently forcing a stretch on the active spasm, micro-tearing already fragile, electrolyte-stripped muscle fibres. |
Stiff, creaky knees upon standing | Synovial fluid viscosity has increased due to systemic dehydration; cartilage is absorbing less fluid, increasing articular surface friction - the joint is grinding bone-adjacent tissue. | Taking an NSAID and sitting back down. Immobility stops synovial circulation entirely. |
Tension headaches traveling down the neck | Thermal shock from AC-to-street transitions is triggering trapezius and levator scapulae spasm. The suboccipital muscles are locked, referring pain forward through the trigeminal pathway. | Blasting cold air directly onto a sweat-drenched neck. This is not cooling; this is a fascial assault. |
Heavy “cement” legs | Profound cellular dehydration causing ischaemic pain in the posterior chain - reduced plasma volume means less oxygen-carrying blood reaching the gastrocnemius and soleus. | Dismissing it as tiredness and lying still for hours, allowing venous pooling and compounding the muscular hypoxia. |
The Biomechanics of 50°C: What Extreme Heat Does to Your Body, Tissue by Tissue
Extreme heat does not just make you uncomfortable. It chemically and mechanically alters your connective tissue, degrades your joint environment, and triggers a cascade of neuromuscular failures that a painkiller cannot reach. Here is exactly what is happening inside your body.
1. The Fascial Drought: Why Your Connective Tissue Stiffens Like Beef Jerky
Fascia - the dense, collagen-rich web of connective tissue that wraps every muscle, organ, and bone in your body - is approximately 68% water by composition. When you are sweating at the rate Karachi’s heat demands (easily 1–2 litres per hour during physical activity), you are not just losing fluid. You are desiccating your fascia. As fascial hydration drops, the ground substance - the viscous gel matrix that keeps collagen fibres gliding past each other - thickens and loses pliability.
You feel it in the back of your body: that deep, unyielding tightness from the base of your skull, down through the lumbar fascia, and into the plantar fascia of the foot. What used to be a glide is now a rip. That is not a metaphor. At severe levels of fascial dehydration, rapid stretching can cause micro-tears in already brittle collagen structures. This is why aggressive yoga or ‘stretching it out’ during a heatwave, without first fully rehydrating, is genuinely dangerous. Drink first. Wait. Then move slowly and with intention.
The counter-measure is not just water. It is electrolyte-rich oral rehydration - sodium, potassium, and magnesium - taken incrementally over hours, followed by slow, non-ballistic fascial mobilisation: foam rolling, gentle joint circles, and diaphragmatic breathing that mechanically pumps fluid back into the fascial planes.
2. Synovial Sludge: How Dehydration Destroys Your Joints Lubrication System
Every moveable joint in your body is enclosed in a synovial capsule filled with synovial fluid - a viscous, nutrient-rich lubricant that reduces articular friction and feeds the avascular cartilage that cannot receive nutrients from blood vessels directly. Under normal conditions, it behaves like a high-grade biological oil. Under dehydration-level conditions, synovial fluid viscosity increases as its hyaluronic acid concentration becomes less dilute. The fluid thickens.
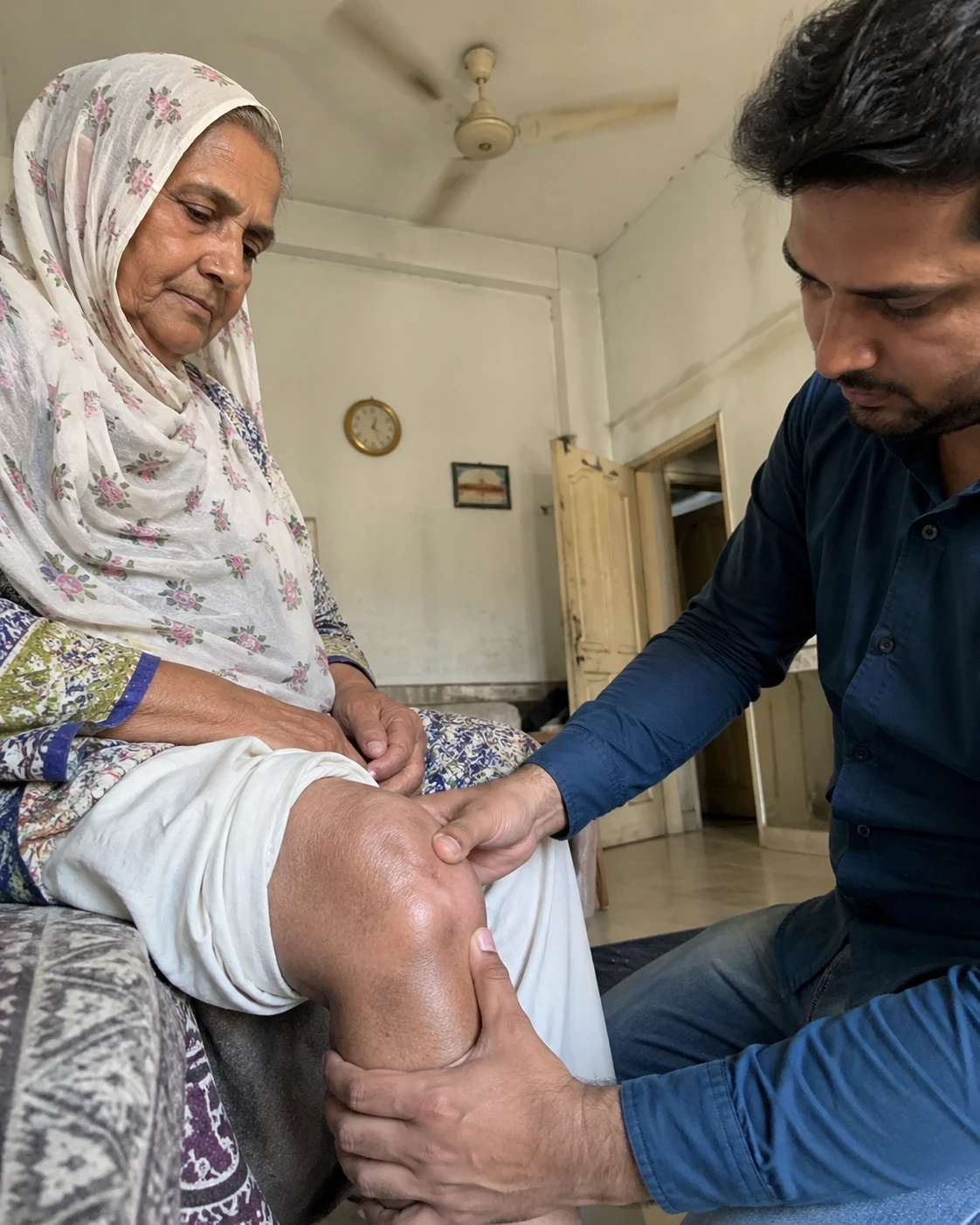
The knee joint is the first casualty. After walking even short distances in 45°C heat - from your car to a building entrance - the joint capsule is already thermally stressed. Cartilage, which relies on fluid absorption for shock absorption, is working with an inadequate supply. The grinding, cracking sensation you feel when you stand up after sitting is not age. It is articular surface friction in a poorly lubricated joint capsule. For patients who already carry an osteoarthritis diagnosis, this is not discomfort - it is an acute flare-up with a measurable duration.
The clinical counter-measure: non-weight-bearing joint cycling. Seated ankle pumps, supine knee-to-chest pulls, and slow hip circles in the morning before you stand for the first time - these actions mechanically pump fresh synovial fluid across the articular surfaces. Two minutes. Every morning. Before your feet hit the floor. This is not optional if you are arthritic and living through a Karachi summer.
3. The AC Trap: How Thermal Shock Triggers Instant Muscle Spasm
Stop blasting your AC at 16°C directly onto your sweat-drenched neck the second you get home. You are not cooling down; you are forcing your trapezius into a violent, locked spasm. You need gradual cooling, not a thermal shock to your fascia.
Here is the physiology: when you step from a 45°C street into an 18°C room, the sudden drop in ambient temperature triggers an involuntary protective response in the peripheral musculature. Cutaneous thermoreceptors fire. The sympathetic nervous system instructs the superficial muscles - predominantly the trapezius, sternocleidomastoid, and cervical erectors - to contract to conserve core heat. This is not voluntary. The muscles do not ask your permission. If those muscles are already fatigued and electrolyte-depleted from hours of heat exposure, they can enter a sustained, painful spasm from which they will not release without manual intervention.
This is the direct cause of the brutal tension headaches that travel from the base of the skull forward - cervicogenic referred pain from a trapezius in sustained tetanic contraction. The counter-measure is absolute: enter a cool space gradually. Remove yourself from direct AC flow. Wet a cloth with room-temperature water and apply it to the back of the neck first. Give your peripheral vasculature 10 minutes to begin equilibrating before sitting under a vent. You are protecting your fascia, not being dramatic.
4. Electrolytes vs. Biomechanics: Why Stretching a Sodium-Depleted Muscle Tears It
This is the most dangerous thing most Karachi households get wrong. A muscle cramp triggered by hyponatremia - critically low serum sodium - is not a mechanical tightness. It is a neurochemical failure. The sarcoplasmic reticulum cannot complete its calcium reuptake cycle because sodium-potassium pump activity is compromised. The muscle fibre is locked in contraction at a cellular level.
Stretching that muscle - aggressively, as most people’s instinct dictates - does not address the sodium deficiency. It applies tensile force to a fibre that is already generating its maximum internal force. The outcome is predictable and grim: micro-tears in the myofibril bundles, delayed onset muscle soreness, and bruising within the fascial sheath. The cramp releases temporarily from stretch reflex inhibition and then immediately re-locks.
The correct clinical sequence is: hydrate first. A sachet of WHO-formula ORS dissolved in 200mL of water. Wait 8–10 minutes. Only then apply gentle reciprocal inhibition - contract the opposing muscle group to neurologically inhibit the cramping one. For a calf cramp: dorsiflex the foot by pulling the toes toward the shin while keeping the knee straight. Do not force it. The sodium has to arrive at the cell before the biomechanics can work.
5. The Desk-Bound Heat Trap: How Load-Shedding and Slumped Posture Destroy Your Lower Back
Four hours of load-shedding in Karachi in June means four hours of sitting in a sweat-soaked chair with no fan, no AC, progressively wilting into a posterior pelvic tilt as your core fatigues and your discs compress. The lumbar intervertebral discs are also largely avascular - they receive nutrition through diffusion and movement. Sustained, static, heat-compromised sitting switches that nutrient exchange off entirely.
Add to this the dehydration-induced reduction in disc height - the nucleus pulposus loses fluid under load - and you have the physiological foundation for the heavy, cement-like lower back fatigue that patients describe when I visit them in the evening after a long, hot, load-shedding day. It is not muscular fatigue alone. It is discogenic and fascial compression that has been building for hours with no mechanical relief.
The counter-measure is a strict interruption protocol: every 45 minutes of sitting, you stand and perform 10 repetitions of lumbar segmental extension - hands on the lower back, gently arching backward to restore disc height and pump fluid exchange back into the posterior annulus. This takes 90 seconds. It is the difference between a manageable day and a back that will not let you sleep.

The Fatal Heatwave Musculoskeletal Mistakes
Aggressively forcing a stretch on an actively cramping muscle. A hyponatremia-induced spasm is not mechanical tightness - it is a cellular electrochemical lock. Applying ballistic tensile force to a fibre that is already at maximum internal contraction does not release it; it tears the myofibril bundles and causes secondary delayed onset muscle soreness that can last a week.
Taking NSAIDs (ibuprofen, diclofenac) for heat-induced muscle cramps instead of immediately drinking ORS. NSAIDs address prostaglandin-mediated inflammation - they have zero mechanism of action on sodium depletion-driven neuromuscular failure. They also carry a documented acute kidney injury risk during heat stress and dehydration, when renal perfusion is already compromised. You are adding organ risk for zero musculoskeletal benefit.
Sitting completely still during a heatwave. Zero movement means zero synovial fluid circulation. Cartilage in a static joint receives no nutritional exchange. Venous pooling compounds the ischaemic pain in the lower extremities. Even two minutes of ankle pumping and seated marching every hour changes the joint environment fundamentally.
Drinking only plain water during a heatwave. Hyponatremia - dangerously low serum sodium - can be induced by drinking excessive plain water without replacing lost electrolytes. The result is paradoxical worsening of cramps despite apparent rehydration. ORS formulation exists precisely for this scenario.
Ignoring joint stiffness as ‘just age.’ A stiff, grinding knee in a 55-year-old Karachi patient during May–June is not simply osteoarthritis on autopilot. It is an arthritis flare triggered by a specific, reversible mechanism: synovial fluid degradation under dehydration. It has a clinical counter-measure. Dismissing it as inevitable ageing costs weeks of function.
Extreme Heat FAQs
Why do my legs cramp so violently at night during the summer in Karachi?
Nocturnal leg cramps during summer are almost always driven by electrolyte depletion accumulated over the day, not a single event. Throughout the day, sweating strips sodium, potassium, and magnesium from your extracellular fluid. At night, when your muscles reach their resting tone and your sarcoplasmic reticulum attempts its calcium reuptake cycle, the sodium-potassium pump does not have adequate substrate to complete the process. The muscle fibre cannot relax and locks into a tetanic cramp. The solution is aggressive afternoon ORS intake and a magnesium-rich meal - lentils, leafy greens - before sleeping.
How does dehydration from extreme heat affect my arthritis and knee pain?
Cartilage has no direct blood supply - it receives all its nutrition and hydration through diffusion from synovial fluid. Under systemic dehydration, synovial fluid volume decreases and viscosity increases, meaning cartilage receives less fluid exchange with every loading cycle. The articular surfaces begin experiencing increased friction and inadequate shock absorption - the biomechanical definition of an arthritis flare-up. Rehydrating over 4–6 hours and performing non-weight-bearing joint cycling will measurably reduce this friction within 24 hours.
What is the safest way to stop a severe heat-induced muscle spasm at home?
Begin with hydration: one sachet of WHO-formula oral rehydration salts in 200mL of water, consumed slowly. Wait 8 minutes - this is not negotiable, because no mechanical technique will work on a sodium-depleted fibre. Then apply reciprocal inhibition: contract the antagonist muscle to neurologically suppress the cramping one. For a calf cramp, actively dorsiflex the ankle, pulling the toes toward the shin, using your anterior tibialis to inhibit the gastrocnemius. Hold for 30 seconds. Repeat. Do not force a passive stretch until the electrolyte cycle has had time to partially restore.
The 2015 Echo: Building Physical Resilience for 2026
In June 2015, Karachi experienced a heatwave that killed more than 1,200 people in under a week. The death toll received global attention. What received almost none was what happened to the survivors in the months that followed.
I was not yet studying physiotherapy in 2015. But the clinical picture has been well documented by elders and seniors who were: patients who survived the heatstroke were left with severe, persistent musculoskeletal sequelae - profound generalised weakness, frozen hip and shoulder joints from extended hospitalisation in fixed positions, lower limb muscle atrophy from sustained immobility, and chronic lower back pain from weeks of bed rest on inadequate surfaces. Some required months of physiotherapy to regain walking function. Others never fully recovered their pre-event strength baseline.
The Super El Niño 2026 Karachi forecast is no longer speculative. The PMD projections are consistent with the National Oceanic and Atmospheric Administration’s El Niño outlook. And the lesson from 2015 is not just "drink water and find shade." It is that your musculoskeletal system needs active preparation - now, before the peak temperatures arrive. Not after.
That means building your joint health, your fascial hydration, and your electrolyte management discipline in April and May - so that when the 48°C days arrive in June, your cartilage is not already running on a deficit, your fascia has adequate ground substance to resist thermal stiffening, and your muscles have the neuromuscular reserves to resist cramping under dehydration load. This is exactly what Karachi physiotherapy at home through Sehat Door is designed to deliver: structured, clinical home assessments that evaluate your joint health, postural risk factors, and electrolyte management strategies before the crisis hits - not during it.
The physiotherapy patients we see after a heatwave look like trauma patients: atrophied, frozen, and frightened. What keeps you off that list is not luck. It is not painkillers. It is deliberate, consistent, biomechanically-informed movement - and the knowledge of exactly what your body is doing, tissue by tissue, when the temperature crosses 45°C. Now you have that knowledge.
If you are already noticing stiffness, deep joint aches, or recurring cramps this season, do not wait for it to escalate. Search for heatwave muscle cramp relief or reach out for a Sehat Door at-home physiotherapy assessment now - before May-June turns Karachi into a place where getting up from a chair becomes the most painful part of your day.
The most dangerous thing you can do in a Karachi heatwave is nothing. Immobility is not rest. Stillness is not recovery. Every hour you sit locked in a slumped, dehydrated posture without movement is an hour your discs are compressing, your cartilage is drying, your fascia is stiffening, and your muscles are loading up the sodium deficit that will detonate in your calf at 2 AM while your family sleeps. Your joints are not failing you. You are failing them. And that is entirely, clinically reversible - but only if you act before the damage compounds.
DISCLAIMER: This article is for preventative educational purposes only and does not constitute individual medical advice. If you or a family member are experiencing symptoms of heatstroke - including cessation of sweating, confusion, or loss of consciousness - seek emergency medical care immediately.

Dr. Aleena PT
A Physiotherapy Doctor (DPT) from Jinnah Sindh Medical University, focused on musculoskeletal rehabilitation, evidence-based patient care, pain management, mobility improvement, and recovery support.